Next Generation NCLEX Background
In the modern era, where healthcare practices are becoming more challenging, nurses are required a more advanced approach to fulfill the requirements of client needs.
In 2013 and 2014 National Council of State Boards of Nursing (NCSBN) performed a detailed analysis known as “NCSBN Strategic Practice Analysis” on nurses’ knowledge and skills for improvement in nursing practices and to identify the minimal level of nurses’ knowledge and skills mandatory for nursing practices.
The main and most important finding of this analysis was that there was a gap between the current nursing practice and the knowledge and skills required for safe, competent, and ethical practice.
This gap has been identified as a major concern by NCSBN and other stakeholders in the healthcare industry. On April 1st, 2023 NCSBN launched the Next Generation NCLEX-RN (NGN) Exam for newly graduated nurses, which is based on the NCSBN Clinical Judgment Measurement Model (NCJMM).
This model helps nurses to build up their critical thinking and decision-making by identifying their strengths and weaknesses and evaluating the solutions.
The NCJMM is comprised of six measurable cognitive skills which are the basic elements of nursing practice including recognizing cues, analyzing cues, prioritizing hypotheses, generating solutions, taking actions, and evaluating outcomes.
Is the New NCLEX Easier?
NGN is not a different or separate examination. It is an advanced version of the current NCLEX-RN Exam which assures a better measurement of the clinical judgment of nurses. NGN is launched with a new methodology of scoring, and changes in test length with the addition of NGN item types.
- Part A: The first part of the test is the same as the current NCLEX-RN exam, which consists of 250 questions that are divided into four categories: psychomotor skills, cognitive skills, affective behaviors, and communication and interpersonal skills.
- Part B: This part will be added to the current examination to measure clinical judgment.
- Part C: This part is similar to the current NCLEX-RN exam and consists of questions that evaluate your ability to apply nursing knowledge and skills.
What is the NCSBN Clinical Judgment Measurement Model?
The model of Clinical Judgment Measurement is based on the six cognitive skills to measure the critical thinking and decision-making of nurses in clinical practices. These cognitive skills include:
Recognize Cues:
This cognitive skill make nurses enable to identify the most essential data in question. The cues are the client’s current and previous findings and assessment data that lead nurses to make decisions in a clinical environment.
In unfolding case studies you will be given a scenario and you need to find out the more relevant information which is directly related to the client’s clinical needs and priorities or you need to identify the irrelevant information which is not directly related to the client’s needs and priorities.
Analyze Cues:
Analysis of cues, help nurses to find out the actual or potential meaning of all the data. This cognitive skill guides nurses to identify the most immediate concerns and priority actions in a clinical setup.
In some scenarios, you can find out more than one client’s condition then you need to link the conditions to identify the most concerning condition and plan your nursing care as per the client’s need.
In some cases, there could be some potential complications rather than actual which can affect the client’s condition in the future. Identify those conditions and anticipate possible complications and prioritize client care accordingly.
Prioritize:
The center of your nursing practice is that you need to anticipate and make hypotheses about the priority needs and take decisions in more complex situations according to client needs and problems. In this cognitive skill, you review the client’s problems and needs and link them with the client’s actual or potential conditions.
After all, you make a hypothesis about the prioritization of client needs and you perform the most crucial and necessary step first. Consider this clinical scenario.
A 43-year-old client presents in the emergency department complaining of loose stool 20 episodes from the previous day, vomiting, and abdominal pain. On examination nurse notes a low blood pressure of 100/60 mmHg.
What the nurse will anticipate priority action according to the client’s actual or potential clinical condition. In this scenario, the patient has four main problems loose stool, vomiting, abdominal pain, and low blood pressure. What could be the most alarming problem that the nurse should anticipate to treat first?
- Start intravenous fluids.
- Administer pain medicines.
- Administer antibiotics.
- Provide oral rehydration solution.
In this scenario, the alarming potential condition is that the patient can develop hypovolemia which can be life-threatening. So the first action of the nurse should start intravenous fluids.
The patient is not tolerating oral fluids so the oral rehydration solution should be avoided. Low blood pressure and abdominal pain are related to low body fluid volume, electrolyte imbalance, and smooth muscles spasm. They all can be treated after starting the intravenous fluids.
Generate Solutions:
In this cognitive skill, nurses develop a plan of care by anticipating client needs and actual or potential conditions. Nurses rank the priority actions on evidence-based nursing interventions and solutions for client safety by providing safe delivery of nursing care.
When making a plan of care for Generate Solutions you need to identify the outcome criteria on the client’s priority needs. Nurses should know when they are required to Generate Solutions.
Nurses should consider themselves as problem solver and should make a hypothesis based on current condition, actual and potential risk, prioritizing client needs and revising the plan of care if needed.
- To identify the current condition efficiently.
- To identify the actual and potential risks for client health and safety.
- To prioritize the client’s needs.
- To make a hypothesis.
- To develop a plan of care.
- To evaluate the plan of care.
Take Action:
Making a plan of care and generating solutions guide the nurses to take action accordingly. Implementation of nursing actions is a practical approach to evaluating a plan of care. Undertaking necessary actions can prevent the client’s deterioration and improve the client’s health.
To maintain safe client care nurses must be able to use their clinical judgment according to the client’s health status. In critical situations, nursing knowledge and clinical judgment play an important role to take action immediately and effectively.
- C= Clinical condition of the client provides a broad view of the current situation, so nurses should assess the clinical condition of the client very carefully.
- R= Recognizing the cues, client’s clinical history and assessment data provides the base to make a care plan for nurses.
- I= Investigations guide the nurses about actual and potential risks and problems.
- T= Critical thinking is the most important factor in the assessment, prioritization of client needs, planning, and implementation of nursing actions.
- I= Initiate the nursing actions to execute the plan of care.
- C= Collect the data after initiation of the care plan.
- A= Analysis of findings and collected data help nurse to make an evaluation and to make a better judgment that nursing interventions worked or not,
- L= List all the collected data and make an evolution. This determines that the how care plan was effective. Your outcome goals are achieved or you need to modify your care plan.
Evaluate Outcomes:
Evaluation of outcomes is the process of determining whether your care plan is effective or not. This is an ongoing process that helps nurses to look back on all the steps for the continuation or modification of the nursing care plan.
Nurses set their expected outcome goals and compare them with actual client outcomes and make an evaluation for the care plan. This cognitive skill requires good communication skills to identify the client’s findings, document of client’s response, and report the client’s findings, response, and investigations in the care plan.
Evaluate Outcome Cognitive skill guide nurses to move forward or to revise their nursing care plan according to client response and actual outcome goals.
- Client’s previous and current condition.
- Any change in the client’s condition.
- Factors influencing the care plan.
- Is there any new client need if so prioritize according to the client’s needs.
- What else needs to be done to achieve optimal results?
- The care plan is effective or needs to be revised based on client needs.
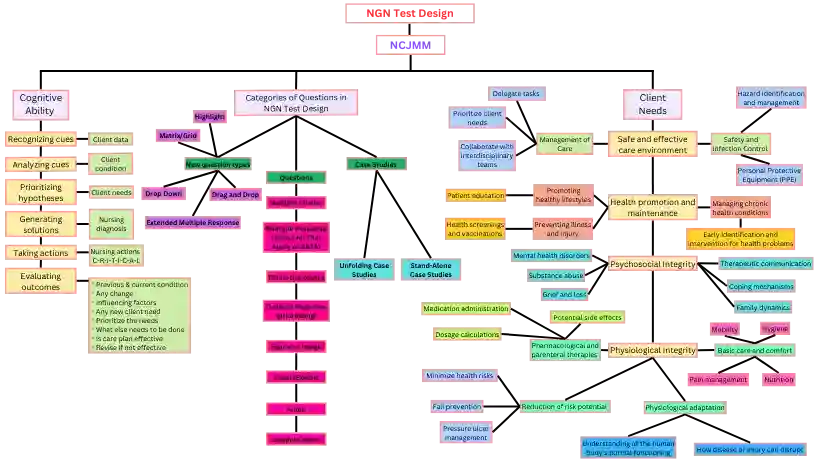
Structure of the Next Generation NCLEX (NGN) Exam
The Next Generation NCLEX (NGN) Exam is a comprehensive test designed to assess the knowledge and skills of nurses. It is used to measure the competence level of nurses to ensure they are qualified for their roles.

The exam is structured in a way that allows nurses to demonstrate their expertise in various areas such as medical-surgical nursing, pharmacology, and mental health nursing.
The NGN exam also includes questions related to patient safety, communication, and professionalism. This structure ensures that all nurses are evaluated on the same criteria and can effectively demonstrate their knowledge.
The Next Generation NCLEX (NGN) Test Design is an important exam for nurses to be able to practice in the United States. It provides a framework for understanding the knowledge, skills, and abilities that are necessary for registered nurses to have to provide quality patient care.
The NGN is an updated version of the traditional NCLEX, developed by the National Council of State Boards of Nursing (NCSBN). This new test design went into effect on April 1, 2023, and represents a significant shift in assessing nursing candidates’ clinical judgment and cognitive abilities.
The NGN aims to better prepare nursing professionals for real-world clinical situations by focusing on clinical judgment, decision-making, and critical thinking skills. Following are the components of the Next Generation NCLEX (NGN) Exam.
1. Cognitive Ability in the NGN Test Design
- Recognizing cues
- Analyzing cues
- Prioritizing hypotheses
- Generating solutions
- Taking actions
- Evaluating outcomes
By evaluating these cognitive abilities, the NGN ensures that nursing candidates are well-equipped to make informed clinical judgments and provide high-quality care in various healthcare settings.
2. Client Needs in the NGN Test Design
The NGN test design is structured around four main categories of client needs, which are essential for nursing professionals to understand and address effectively. These categories include:
- Safe and Effective Care Environment
- Health Promotion and Maintenance
- Psychosocial Integrity
- Physiological Integrity
Each category encompasses a wide range of nursing topics, ensuring that nursing candidates possess the knowledge and skills necessary to provide safe, effective care across diverse patient populations and healthcare settings.
3. Safe and Effective Care Environment
The Safe and Effective Care Environment category is weighted at 25-37% in the NGN test design. This category focuses on the ability of nursing professionals to provide safe and effective care in various settings. It is divided into two sub-categories:
Management of Care (15-21%): This sub-category assesses a candidate’s ability to prioritize patient needs, delegate tasks to other healthcare professionals, and collaborate with interdisciplinary teams to develop and implement care plans.
Safety and Infection Control (10-16%): This sub-category evaluates a candidate’s understanding of infection control measures, personal protective equipment (PPE) usage, hazard identification and management, and other critical aspects of maintaining a safe healthcare environment.
4. Health Promotion and Maintenance
Health Promotion and Maintenance are weighted at 6-12% in the NGN test design. This category emphasizes the importance of nursing professionals in promoting healthy lifestyles, preventing illness and injury, and managing chronic health conditions. Key topics within this category include:
- Patient education on healthy behaviors.
- Health screenings and vaccinations.
- Early identification and intervention for health problems.
5. Psychosocial Integrity
The Psychosocial Integrity category carries a 6-12% weight in the NGN test design. This category assesses candidates’ knowledge and abilities in treating patients with mental health and psychosocial problems. Important topics within this category include:
- Therapeutic communication.
- Coping mechanisms.
- Mental health disorders.
- Substance abuse.
- Grief and loss.
- Family dynamics.
6. Physiological Integrity
Physiological Integrity is weighted at 33-57% in the NGN test design and is broken down into four subcategories:
Basic Care and Comfort (6-12%): This sub-category covers essential nursing care, including hygiene, mobility, nutrition, and pain management.
Pharmacological and Parenteral Therapies (13-19%): This sub-category assesses candidates’ knowledge of medication administration, dosage calculations, and potential side effects.
Reduction of Risk Potential (9-15%): This sub-category focuses on nursing interventions that minimize health risks, such as fall prevention and pressure ulcer management.
Physiological Adaptation (11-17%): This sub-category evaluates candidates’ understanding of the human body’s normal functioning and how disease or injury can disrupt these processes.
Categories of Questions in the NGN Test Design
The NGN test design features a diverse range of question types to ensure a comprehensive assessment of nursing candidates’ knowledge and skills. Question categories include:

- Multiple Choice Questions.
- Multiple Response (Select All That Apply or SATA).
- Fill-in-the-blanks.
- Ordered Response (prioritizing).
- Figure or Image.
- Chart/Exhibit.
- Audio.
- Graphic Option.
Additionally, the NGN introduces several new question types, such as:
- Highlight
- Drag and Drop
- Drop Down
- Matrix/Grid
- Extended Multiple Response
- Extended Multiple Choice questions
These innovative question types are designed to better assess candidates’ clinical judgment and decision-making abilities, reflecting real-world nursing situations.
Case Studies in the NGN Test Design
The NGN test design incorporates case studies to provide candidates with realistic clinical scenarios that mirror the challenges they may face in their nursing practice. There are two types of case studies in the NGN:
Unfolding Case Studies:
These case studies present a clinical situation that evolves, with accompanying questions that measure each of the six cognitive skills.
Stand-Alone Case Studies:
These case studies include the Bowtie and Trend types, which present clinical situations at a single point in time or require a review of information over time to measure one or more cognitive skills.
Prepare for the Next Generation NCLEX
Exam Administration and Scoring
The NGN is administered using a computerized adaptive testing (CAT) format, which selects questions based on candidates’ responses to previous questions. This ensures a unique and customized examination experience for each candidate.
Partial credit scoring is available for some items on the NGN, including SATA questions. The NGN test design also provides reference ranges for laboratory tests, eliminating the need for candidates to memorize lab values.
Preparing for the NGN Test
To prepare for the NGN, candidates should practice a variety of traditional and NGN-style questions, focusing on understanding rationales and test-taking strategies.
Resources such as the Saunders Comprehensive Review books, Q&A books, and Clinical Judgment and Test-Taking Strategies book can be invaluable in helping candidates prepare for this critical examination.
Conclusion
The Next Generation NCLEX (NGN) test design represents a significant evolution in nursing licensure examinations, with a focus on cognitive ability, client needs, and innovative question types.
By understanding the structure and content of the NGN, nursing candidates can better prepare themselves for this critical examination and excel in their nursing careers.
References:
- Silvestri, L.A., Silvestri, A.E. and Ignatavicius, D.D., 2022. Strategies for Student Success on the Next Generation NCLEX®(NGN) Test Items-E-Book. Elsevier Health Sciences.
- NCSBN launches Next Generation Nclex Exam (04/03/2023) NCSBN. Available at: https://www.ncsbn.org/news/ncsbn-launches-next-generation-nclex-exam (Accessed: April 25, 2023).
- What to know about next generation NCLEX® (2023) UWorld Nursing. Available at: https://nursing.uworld.com/educators/next-gen-nclex/ (Accessed: April 25, 2023).