What are ethical and legal issues?
Ethical issues and legal issues are two distinct but often interconnected aspects that individuals and organizations must address in their daily proceedings while ethical principles in nursing practice are the base of moral ground.
Ethical issues refer to the problems or situations that require a person or organization to decide between alternatives that must be evaluated as right or wrong, ethical or unethical. Ethical issues often arise when the right course of action is unclear or when the interests of different stakeholders conflict.
On the other hand, legal issues refer to situations where the law dictates the course of action. These entail aspects that are governed by established laws and regulations, and failure to adhere to these legal provisions can result in penalties or legal action.
Legal issues usually have a clear course of action as they are guided by written laws and statutes. In many cases, these two types of issues intersect, creating a complex situation where both ethical and legal considerations must be taken into account.
Differences between ethical and legal issues
When making decisions, individuals and organizations often encounter ethical and legal dilemmas. It is important to consider both aspects and make lawful and responsible choices.
Addressing both dimensions ensures a comprehensive approach to decision-making in different contexts. For example, a business can encounter legal problems if it fails to comply with contractual obligations. This, in turn, raises ethical concerns about trust and responsibility.
| Issues | Definition | Nature | Resolution | Examples |
|---|---|---|---|---|
| Ethical Issues | Ethical issues pertain to moral principles and values that guide human behavior and decision-making. They involve considerations of right and wrong, fairness, and the impact of actions on individuals and society. | Ethical issues are often subjective and can vary based on cultural, religious, and individual beliefs. They involve questions about what is morally acceptable or unacceptable. | Ethical issues are typically addressed through ethical frameworks and moral reasoning, encouraging individuals to make decisions that align with principles of fairness, honesty, and respect. | · Patient confidentiality in healthcare · Environmental sustainability in business practices · Truthfulness and transparency in communication · Fair treatment and respect for diversity in the workplace |
| Legal Issues | Legal issues involve matters governed by laws and regulations established by a governing authority. These rules are created to maintain order, protect rights, and ensure justice within a society. | Legal issues are more objective and concrete compared to ethical issues. They are defined by statutes, regulations, and court decisions that dictate what is lawful or unlawful. | Legal issues are resolved through legal processes, which may involve courts, regulatory bodies, and enforcement agencies. Legal frameworks provide a structured way to address disputes and enforce compliance with established laws. | · Breach of contract in business · Violation of privacy laws · Criminal activities and their associated penalties Intellectual property infringement |
Ethical issues for nurses
Nurses encounter a range of ethical issues in their daily practice, given the nature of their work in healthcare and the close interactions with patients and their families. Here are some common ethical issues for nurses:
5. End-of-Life Care
Decisions regarding life-sustaining treatments, do-not-resuscitate (DNR) orders, and the withdrawal of life support can be ethically complex. Nurses may face dilemmas in providing appropriate end-of-life care while respecting the wishes of patients and their families.
Nurses often rely on ethical frameworks and codes of conduct established by nursing organizations to guide their decision-making in these and other situations.
Open communication, collaboration with colleagues, and ongoing ethical education are vital for nurses to navigate these challenges while upholding the highest standards of patient care.
What are the ethical principles in nursing?
Ethical principles in nursing that are relevant to nursing practice include non-maleficence, beneficence, autonomy, justice, veracity, and fidelity.
Non-maleficence requires nurses to avoid causing harm to clients, while beneficence requires them to act in the best interests of their clients.
Autonomy refers to the right of clients to make decisions about their care, while justice requires that care be provided fairly and equitably.
- Non-maleficence
- Beneficence
- Autonomy
- Justice
- Veracity
- Fidelity
You May Also Like To Read : The founders of modern nursing
What is the ANA Code of Ethics for Nurses?
The nursing profession often adheres to a code of ethics that provides guidance and principles for ethical practice. The specific code of ethics may vary slightly depending on the nursing organization or country. However, one of the most widely recognized and influential nursing codes is the “Code of Ethics for Nurses” developed by the American Nurses Association (ANA) in the United States.

The American Nurses Association (ANA) code of ethics is a comprehensive guide designed to assist nurses in ethical decision-making. It offers a framework for ethical practice, emphasizing the importance of ethical values, commitments, and obligations in the nursing profession.
Here are the 9 provisions of the ANA Code of Ethics for Nurses:
Provision 3: Advocacy in the patient’s best interest
The third provision outlines the nurse’s obligation to promote, advocate for, and strive to protect the health, safety, and rights of the patient. This includes privacy and confidentiality rights, as well as advocating for patients who are unable or unwilling to advocate for themselves.
Provision 9: Professional organization
The ninth provision of nursing requires nursing associations and their members to uphold nursing values, maintain professional integrity, and integrate principles of social justice into nursing and healthcare policies.
The ANA code of ethics is a crucial resource for nurses that guides their professional conduct and decision-making. Adhering to this code ensures that nurses maintain the highest ethical standards in their practice, which leads to trust, respect, and dignity in all nurse-patient relationships.
What is the ethical dilemma?
An ethical dilemma occurs when a person faces a situation where they have to choose between two or more moral principles that conflict with each other. It is essentially a state of uncertainty or perplexity, especially when it comes to making a decision where one’s actions could potentially violate ethical standards.
This predicament often occurs in professional settings where individuals or groups are faced with a decision that tests their moral compass. For instance, an employee may be asked to perform an action that conflicts with their personal values or principles.
Ethical dilemmas are particularly prevalent in fields such as healthcare, law, and business, where professionals must constantly balance the needs and rights of their clients against their professional responsibilities and the rules of their employers or their profession.

Many factors can contribute to the ethical dilemma such as religious beliefs, cultural values, and ethnicity. An Ethics Committee is an approach to solving ethical dilemmas within the organizations.
The Ethics Committee is responsible for providing ethical consultation to resolve the ethical dilemma. The crux of an ethical dilemma is the difficult choice between two or more options, none of which resolves the situation in a morally satisfactory manner. This means that no matter what course of action is taken, some ethical principle is compromised.
Thus, the decision-maker must weigh the pros and cons of each option and make the best possible choice considering all factors.
Overcoming an ethical dilemma requires a deep understanding of one’s ethical guidelines, critical thinking skills, and often consultation with others to gain different perspectives.
Every ethical dilemma is unique and there’s seldom a one-size-fits-all solution. Hence, while facing an ethical dilemma can be uncomfortable and challenging, it also offers individuals and organizations an opportunity to reaffirm their ethical framework and strengthen their commitment to conducting themselves with integrity.
What are the most common ethical issues encountered by nurses in clinical practice today?
In the contemporary healthcare landscape, nurses often encounter a range of ethical issues in their clinical practice. These ethical dilemmas can greatly impact patient care and nurses’ professional development. Some of the most common ethical issues encountered by nurses in clinical practice today include:
Nurses are placed in a challenging position of balancing the patient’s wishes, the family’s desires, and the medical team’s recommendations. They must navigate through these conflicting perspectives to ensure that the patient’s dignity and comfort are maintained and that the principle of ‘do no harm’ is upheld.
3. Patient Autonomy
Another ethical issue prevalent in nursing practice is patient autonomy. Patients have the right to be informed and make decisions regarding their healthcare.
However, there can be instances where patients may not fully comprehend the complexities of their health condition or the implications of their choices, leading to an ethical dilemma for nurses. They must respect their patients’ autonomy while ensuring that they have adequate understanding and are making informed decisions regarding their care.
Legal issues in nursing
In addition to ethical issues for nurses, nurses are also faced with a range of legal issues that can impact their practice. Nurses must be aware of the laws and regulations that govern their work, as well as the scope of practice for their profession.
You May Also Like To Read : Complete guide about: Historical perspective of nursing
2. Negligence
Malpractice refers to a failure to provide care that meets the appropriate standard of care, while negligence refers to a failure to provide care that meets the expected level of care.
To minimize the risk of malpractice and negligence claims, nurses should ensure that they are providing care that meets the appropriate standard of care and that they are documenting their care appropriately.
Nurses should also be aware of the legal requirements related to informed consent and refusal and should ensure that clients have sufficient information to make informed decisions about their care. The acts of willful omission and willful commission are also known as negligence.
Areas of legal risks in nursing practice
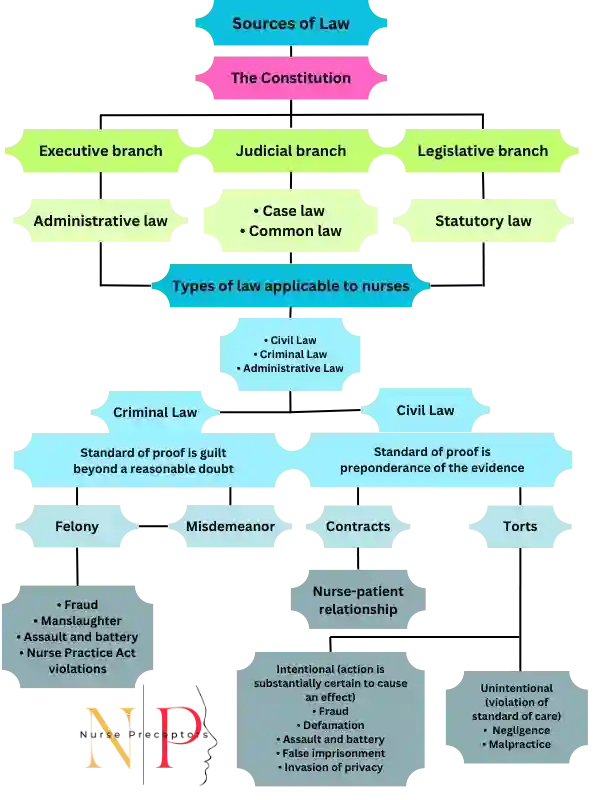
Professional boundaries and relationship in nursing practice
Professional boundaries and relationships are important ethical and legal issues in nursing practice. Nurses must ensure that they are maintaining appropriate boundaries with their clients and that they are not engaging in relationships that could compromise their professional judgment.
To maintain appropriate professional boundaries and relationships, nurses should be aware of the potential risks and benefits of different types of relationships and should avoid engaging in relationships that could compromise their objectivity or judgment.
Nurses should also be aware of the legal and ethical requirements related to professional boundaries and relationships and should seek out support and consultation when faced with difficult situations.
Strategies for addressing ethical issues for nurses and legal issues in nursing
There are a range of strategies that nurses can use to address ethical issues for nurses and legal issues in nursing practice. One important strategy is to stay up-to-date with professional codes and guidelines, as well as the laws and regulations that impact their practice.
Nurses can also seek out continuing education opportunities to improve their knowledge and skills in ethical and legal practice. Many organizations offer free ethics CEUs, which can be a valuable resource for nurses looking to expand their knowledge.
Finally, nurses can seek out support from colleagues and supervisors when faced with difficult ethical or legal dilemmas. Collaboration and consultation can be valuable tool for navigating complex situations and making decisions that are in the best interests of clients.
Conclusion
Non-maleficence in nursing is a key ethical principle that guides nursing practice and is essential to ensuring that clients receive safe and effective care. Nurses are faced with a range of ethical and legal issues in nursing practice, from end-of-life care to client privacy and confidentiality.
By staying up-to-date with professional codes and guidelines, seeking out continuing education opportunities, and collaborating with colleagues and supervisors, nurses can ensure that they are providing care that is aligned with the principles of non-maleficence and other ethical principles in nursing.
References:
- Burkhardt, M.A. and Nathaniel, A.K., 2019. Ethics & issues in contemporary nursing-e-book. Elsevier Health Sciences.
- Pozgar, G.D., 2023. Legal and ethical issues for health professionals. Jones & Bartlett Learning.
- Silvestri, L.A. and Silvestri, A.E., 2019. Saunders Comprehensive Review for the NCLEX-RN® Examination-E-Book.