Do you know that every 30 seconds someone dies in the world from a virus that quietly enters your body and targets one of your most vital organs to make you permanently or temporarily sick?
This is viral hepatitis, a group of infections that cause inflammation of the liver and can lead to severe damage, cancer, and even death.
What is viral hepatitis?
The word “hepatitis” is a combination of two Greek words: “hepar” = liver and “itis” = inflammation. Simply, it’s an inflammation of the liver. But don’t let this simple definition fool you.
The World Health Organization (WHO) estimates that in 2022, about 304 million people were living with hepatitis B and C worldwide. In 2024, the WHO reported that approximately 1.3 million deaths occur globally each year from hepatitis infections.
When we refer to “the group of infections,” it means that this is not a single virus.
What are the types of viral hepatitis?
The 5 types of viral hepatitis are recognized in medical science.
- A
- B
- C
- D
- E
All of these types have the potential to harm liver health. Each one spreads differently, acts differently, affects the body differently, and carries different levels of danger. What makes hepatitis dangerous is how similar it appears in the early stages.
Signs and symptoms of viral hepatitis
According to the Centers for Disease Control and Prevention (CDC), the signs and symptoms of all types of viral hepatitis are generally similar. No matter the type, most people experience symptoms like:
- Nausea
- Fatigue
- Fever
- Stomach pain
- Loss of appetite.
As the disease progresses, more visible signs can appear. Your skin and eyes may turn yellow, a condition called jaundice. Your urine may become dark, and your stools pale or clay-colored.
Diarrhea is a symptom that is specifically associated with hepatitis A infection.
In some cases, individuals may experience significant joint pain and significant tiredness. But sometimes, there are no symptoms at all. Although these infections might appear similar, they differ significantly in terms of transmission, severity, and prevention strategies.
Let’s analyze each type in detail.
Hepatitis A—The food and water infection
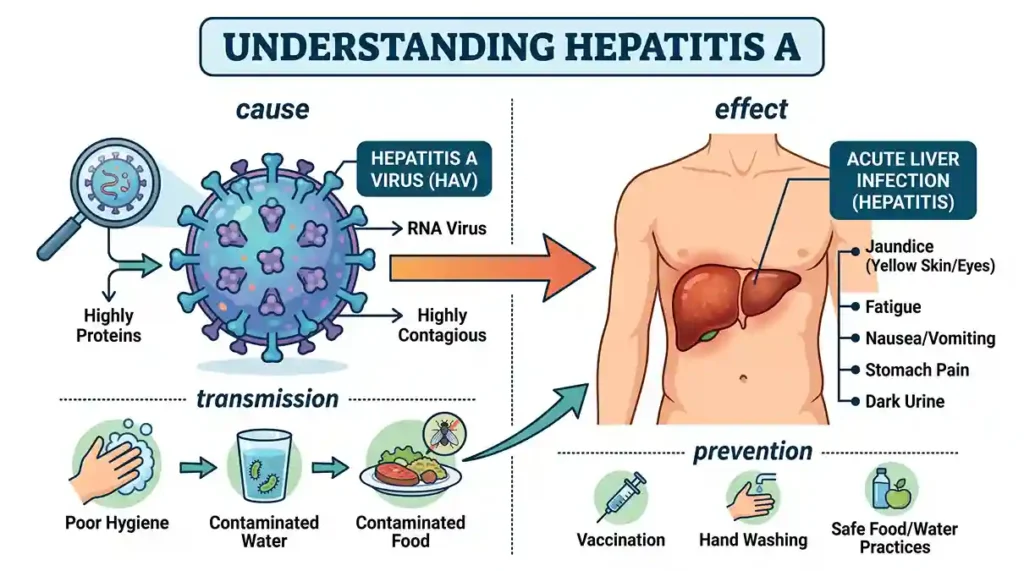
Hepatitis A is a liver inflammation resulting from infection by the hepatitis A virus (HAV). Regions with poor sanitation and hygiene standards are common sites of this virus.
According to the CDC, hepatitis A can also spread through certain types of sexual contact, although the primary route remains contaminated food and water.
The good news is that it does not progress to a chronic state; however, it can still lead to significant illness.
You may be thinking of the regions where hepatitis A is most prevalent. Let’s see that.
Geographical distribution of hepatitis A
Infection rates are higher in low and middle-income countries, where sanitary conditions and hygiene practices may be insufficient. In many developing regions, up to 90% of children get infected before age 10, often without symptoms.
In contrast, infection rates are generally lower in high-income countries that benefit from improved sanitation practices. Recent reports indicate that significant outbreaks have occurred among individuals experiencing homelessness in the United States.
Are you anxious about the treatment of hepatitis A?
What is the treatment of hepatitis A?
Currently, there is no targeted antiviral treatment available for hepatitis A. Management focuses only on supportive care to relieve symptoms and ensure adequate hydration and nutrition. But hepatitis A is preventable.
How to prevent hepatitis A infection?
Preventive measures of hepatitis A are very simple but powerful. Hepatitis A virus can be prevented through:
- Adequate supplies of safe drinking water.
- Proper disposal of sewage within communities.
- Regular hand washing is an essential aspect of personal hygiene.
- It is also important to adopt safer sexual practices.
Several hepatitis A vaccines are available for adults and children worldwide. However, no vaccine is approved for use in children under the age of one year.
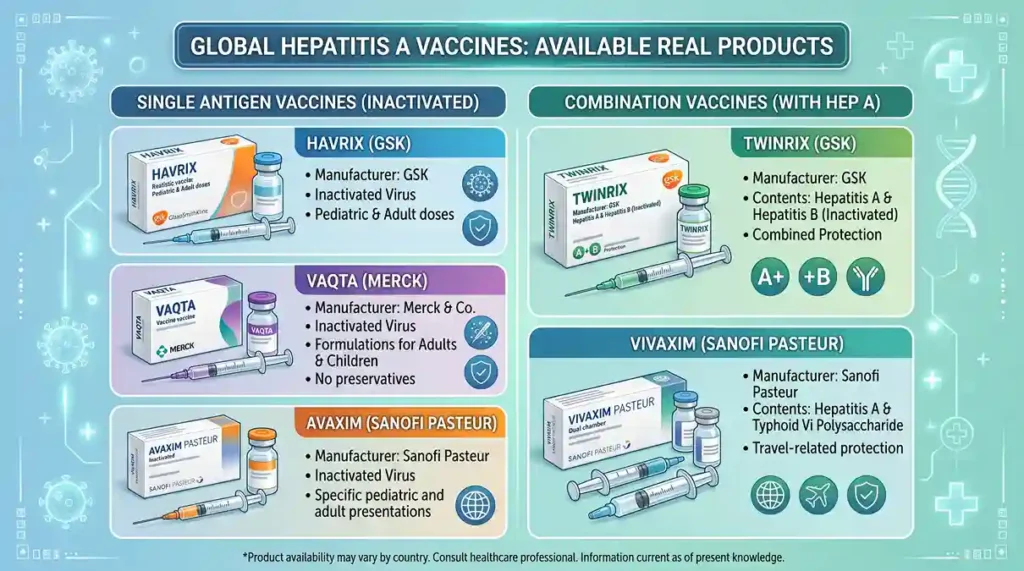
Now, let’s see the second type of hepatitis, which is the most dangerous type.
Hepatitis B—The silent killer
Hepatitis B is a far more serious infection attributed to the hepatitis B virus (HBV). What makes hepatitis B especially dangerous is its ability to become chronic. It can silently stay in the body for years, slowly damaging the liver and eventually putting people at high risk of death from cirrhosis and liver cancer.
The World Health Organization reports almost 1.2 million new infections every year. WHO reported that in 2022, about 254 million people were living with hepatitis B globally, and 1.1 million people died from hepatitis B in the same year.
So, where is this disease more common?
Geographical distribution of hepatitis B
The World Health Organization recognizes hepatitis B as a critical global health challenge.
- The burden of infection is highest in the Western Pacific Region, where 97 million people are infected.
- Secondly, the African Region, where 65 million people are chronically infected.
- In the Southeast Asia Region, about 61 million people are currently affected by infections.
- 15 million in the Eastern Mediterranean Region.
- 11 million in the European Region.
- 5 million in the WHO Region of the Americas.
Let’s explore the mechanisms by which this infection transmits
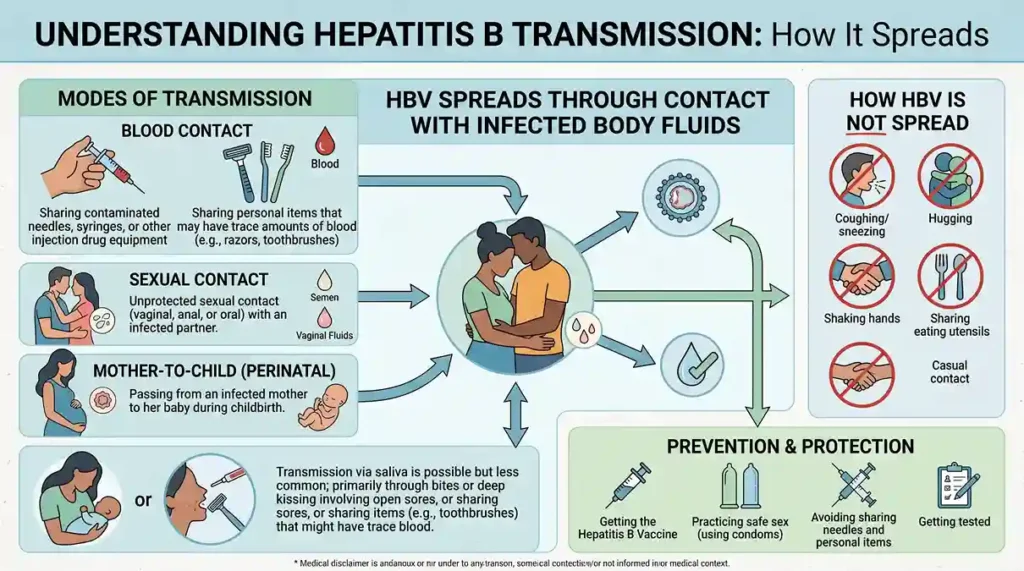
Transmission of hepatitis B
Hepatitis B can spread through contact with the bodily fluids of an infected individual, including blood, semen, and saliva. The routes of transmission include:
- Unsafe injections, such as reusing contaminated needles and syringes.
- Sharing needles among persons who inject drugs.
- From mother to child during childbirth.
- Hepatitis B can be transmitted through needlestick injuries in healthcare environments and may also spread through tattooing and body piercing practices.
- Unvaccinated persons with multiple sexual partners are at high risk of getting hepatitis B during sexual activity.
According to the World Health Organization, acquiring hepatitis B in adulthood becomes chronic in less than 5% of people. Whereas early childhood and infancy are more prone to lead to chronic hepatitis B in almost 95% of children.
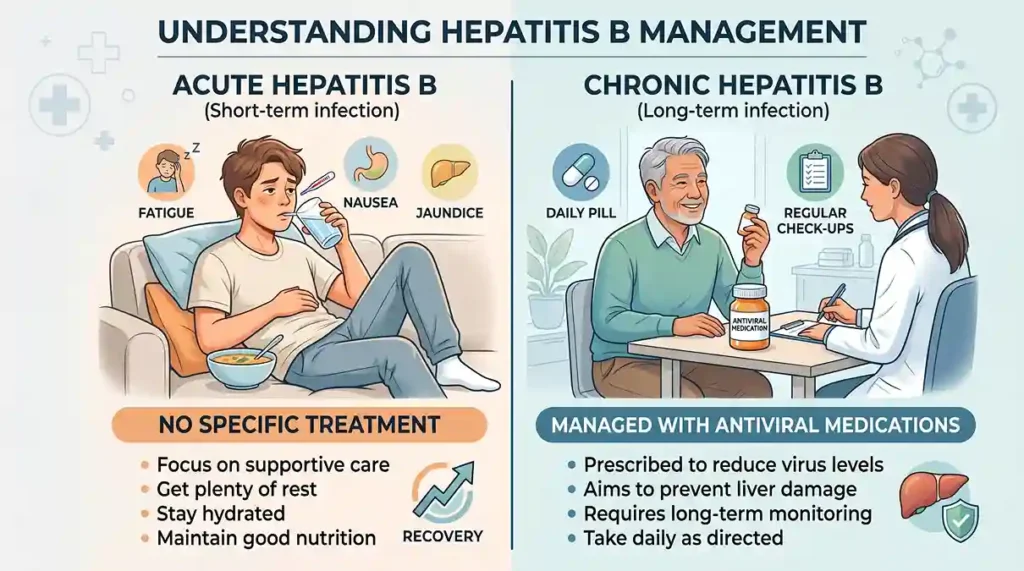
Treatment of hepatitis B
Unfortunately, there is no specific treatment for acute hepatitis B, but in chronic cases, it can be managed with antiviral medications.
Prevention of hepatitis B
HBV can be prevented with vaccination. All babies should receive the hepatitis B vaccine as soon as possible after birth or within 24 hours of birth. The hepatitis B vaccine protects for at least 20 years and is believed to remain effective for a lifetime.
Other preventive measures are:
- Always use condoms for safe sexual activity.
- Never share needles or any other equipment used for injecting drugs, piercing, or tattooing.
- Never recap the syringe needle.
- Wash your hands thoroughly with soap and water after contact with blood or body fluids.
- Receiving the hepatitis B vaccine is strongly advised for individuals working in healthcare settings. This vaccination helps protect both healthcare professionals and patients, ensuring a safer environment for all.
Hepatitis C—The blood-borne disease
Hepatitis C is another major global threat, but with a very different story. It is an infectious disease characterized by inflammation of the liver due to the hepatitis C virus.
Hepatitis C can be acute with mild symptoms or chronic with serious, long-term illness, depending on how early it’s diagnosed and how early you get treatment.
WHO reports that every year, about 1 million new cases of HCV are reported worldwide. At the same time, about 50 million people are currently living with chronic hepatitis C globally. In 2022, about 242000 people died from liver cirrhosis and liver cancer caused by hepatitis C.
Like hepatitis B, it spreads through infected blood. But here’s something different.
Hepatitis C is one of the few chronic viral infections that can actually be cured.
Geographical distribution of hepatitis C
According to the World Health Organization, the highest rate of hepatitis E is in:
- The Eastern Mediterranean Region, where 12 million people are infected with chronic hepatitis C.
- The second-highest occurrence is found in the Southeast Asia Region with 9 million people.
- In the European Region, 9 million people are infected.
- 8 million people are infected in the African Region.
- The burden of this disease in the Western Pacific Region is approximately 7 million people.
- In the Americas, it is around 5 million.
Transmission of hepatitis C
Hepatitis C is primarily transmitted through:
- Reuse of syringes and needles.
- Inadequate sterilization of medical equipment in healthcare facilities.
- Transfusion of untested blood and blood products.
- Sharing of injection equipment between drug users.
- HCV (hepatitis C virus) can be transmitted from an infected mother to her newborn during childbirth.
- It can also be transmitted to people with multiple sexual partners.
Fortunately, hepatitis C does not spread through:
- Breast milk
- Food
- Water
- Hugging
- Kissing
- Sharing food or drinks with someone who is infected with hepatitis C.
What is the treatment of hepatitis C?
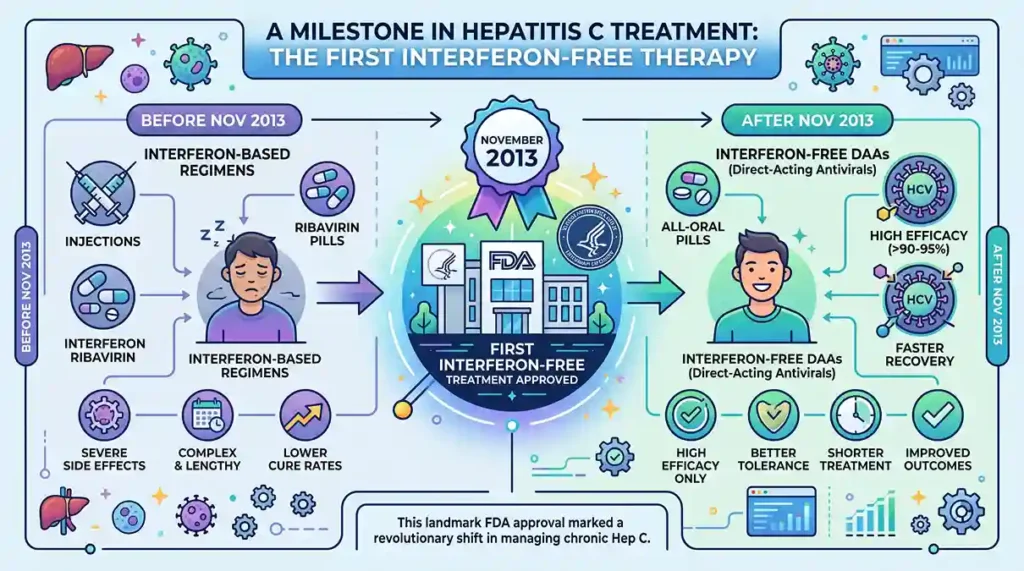
In November 2013, the Food and Drug Administration (FDA) approved the first interferon-free treatment for chronic hepatitis C. This significant development marked a milestone in the management of the disease, offering new hope for patients.
Soon, after this breakthrough, the European Medicines Agency (EMA) also approved the treatment in January 2014. This breakthrough in medicine allowed for a cure in nearly all patients within 8 to 12 weeks of therapy. Today, HCV is treatable and permanently curable in 95% of people without significant signs and symptoms.
The World Health Organization also says that acute HCV mostly does not lead to chronic disease and usually remains asymptomatic. The immune system can naturally clear the infection in about 30% of individuals within six months without treatment.
How to prevent hepatitis C?
Currently, a vaccine for hepatitis C is not available. The recommended preventive measures to mitigate the risk of hepatitis C transmission include:
- Safe usage of injections.
- Performing medical procedures with proper aseptic techniques.
- Proper disposal and safe handling of needles and medical waste are essential.
- Promoting needle exchange programs for drug users.
- Providing counseling to drug users about substance use.
- All donated blood and blood products must undergo comprehensive screening to detect any potential blood-borne diseases.
- Using condoms for safe sexual practices.
Who is at risk of getting HCV?
People at higher risk of getting hepatitis C include:
- Human immunodeficiency virus (HIV) also increases the risk of getting HCV.
- Drug users who share the injection equipment, such as syringes, with other drug users.
- Men who have sex with men.
- Exposure to repeated healthcare procedures, such as hemodialysis.
Now, let’s explore the hepatitis D virus.
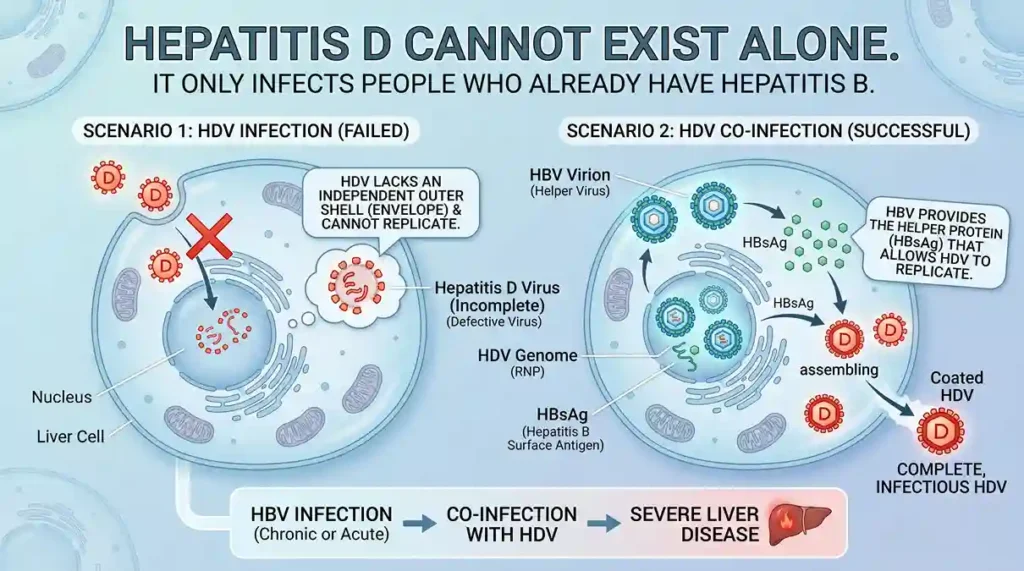
Hepatitis D—The dependent virus
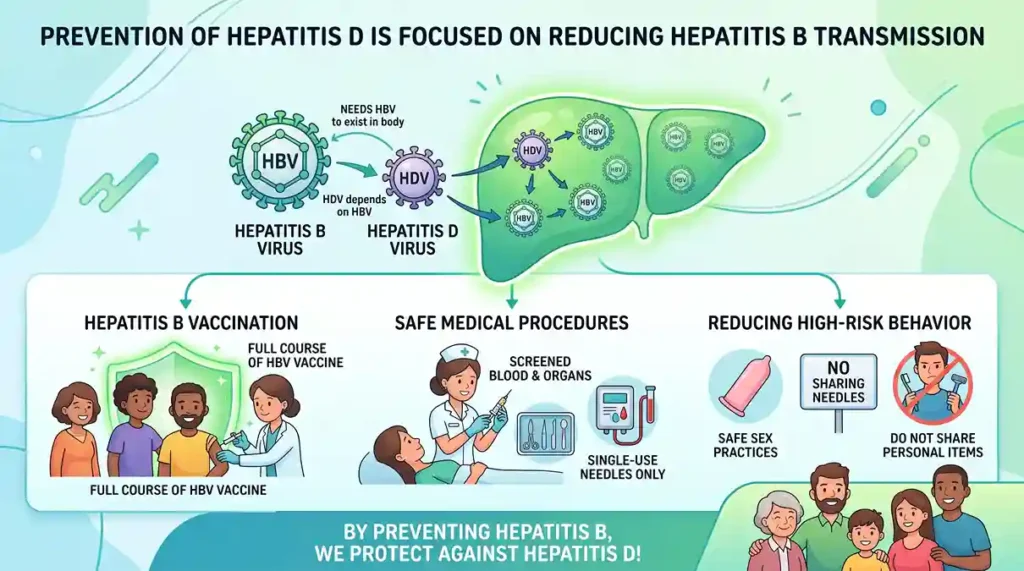
Hepatitis D is also a blood-borne disease caused by the hepatitis D virus (HDV). But this one is different. Hepatitis D cannot exist alone. It only infects people who already have hepatitis B. This means hepatitis D infection cannot occur in the absence of hepatitis B.
Like hepatitis B and C, hepatitis D is also classified as carcinogenic to humans by the International Agency for Research on Cancer (IARC). This indicates that hepatitis D has the potential to cause cancer.
Co-infection of hepatitis B and D is considered the most lethal form of viral hepatitis because it rapidly progresses to hepatocellular carcinoma (HCC), liver cirrhosis, and eventually death.
Geographical distribution of hepatitis D
The World Health Organization (WHO) reports that hepatitis D affects nearly 5% of individuals who have hepatitis B.
Hepatitis D is more prevalent in:
- Mongolia
- The Republic of Moldova
- Western Africa
- Central Africa.
Transmission of hepatitis D
Hepatitis D is transmitted in the same way as hepatitis B.
Transmission can occur through sexual intercourse, and in rare cases, a mother may transmit it to her child either before or during childbirth. The risk of hepatitis D infection may be higher in certain populations, including:
- Recipients of hemodialysis.
- Men having sex with men.
- Commercial sex workers.
What is the treatment of hepatitis D?
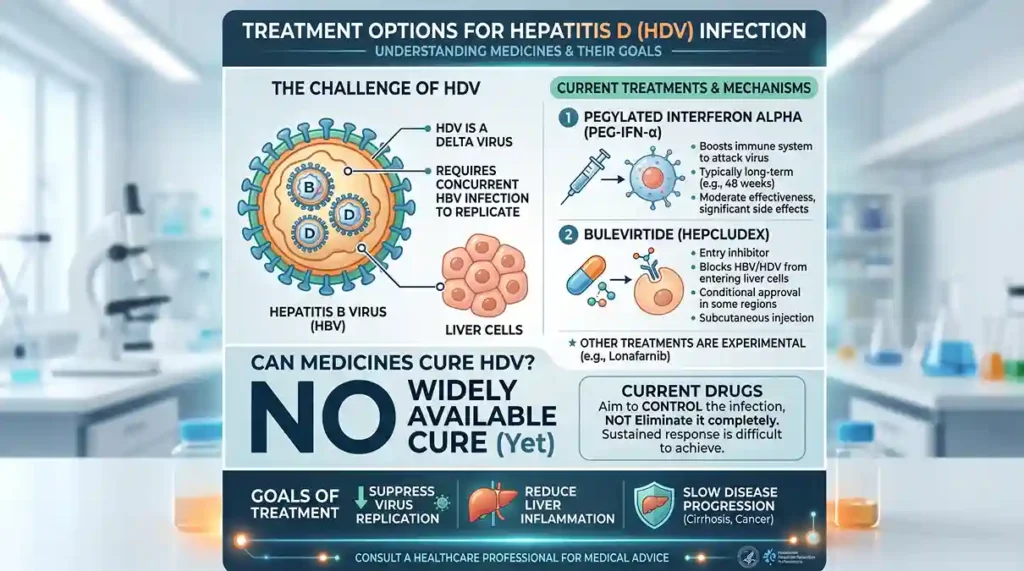
Recent improvements in hepatitis D treatment are providing hope for better management.
The European Medicines Agency (EMA) approved Bulevirtide in 2023. It is a subcutaneous injection for the treatment of chronic hepatitis D in adults who are still in the phase of compensated liver disease.
Multiple centers are evaluating the optimal treatment dosage and duration.
Prevention of hepatitis D
Primary prevention depends on minimizing the transmission of hepatitis B through:
- Immunization or hepatitis B vaccination.
- Providing antiviral prophylaxis for pregnant women who are at risk of developing hepatitis D.
- Blood and blood products screening.
- Safe injection practices in healthcare settings.
- Implementing harm reduction services, including the provision of clean needles and syringes, for individuals who use drugs.
Hepatitis E—The waterborne threat
The hepatitis E virus (HEV) causes the inflammation of the liver. Infected people excrete the virus through their faeces, and it is transmitted to humans via the oral route.
According to the World Health Organization (WHO), approximately 19.47 million people in 2021, across the globe, were living with hepatitis E. 3,450 deaths were also reported worldwide from this infection.
Fulminant hepatitis (acute liver failure) is a critical medical condition that can cause severe and potentially fatal outcomes.
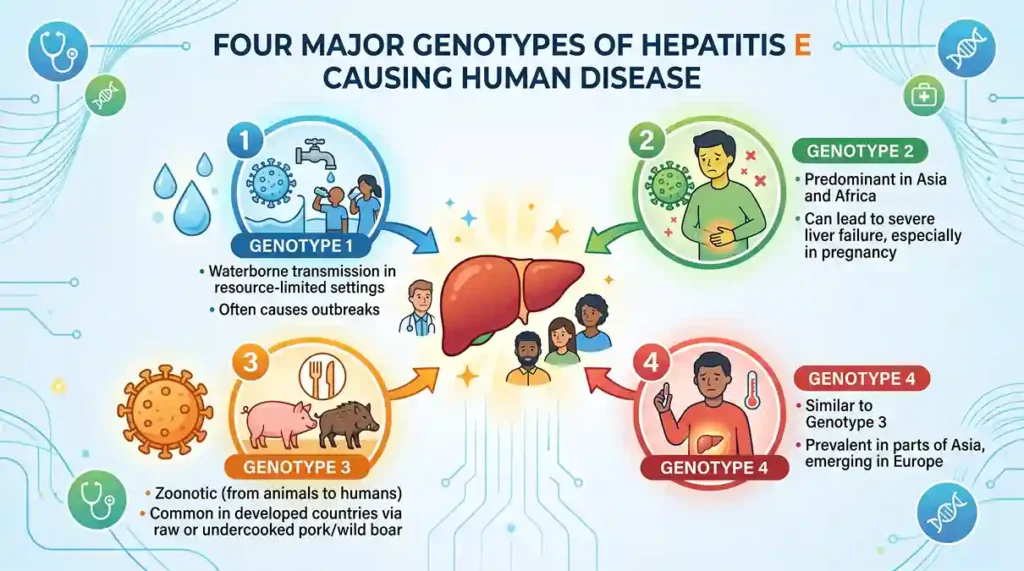
It has four genotypes.
- Genotype 1
- Genotype 2
- Genotype 3
- Genotype 4
Geographical distribution of hepatitis E
Mostly found in low- and middle-income countries that face challenges such as limited access to safe drinking water, inadequate sanitation facilities, and essential health services. Hepatitis E is primarily prevalent in:
- Sub-Saharan Africa
- East Asia
- South Asia
How does hepatitis E spread?
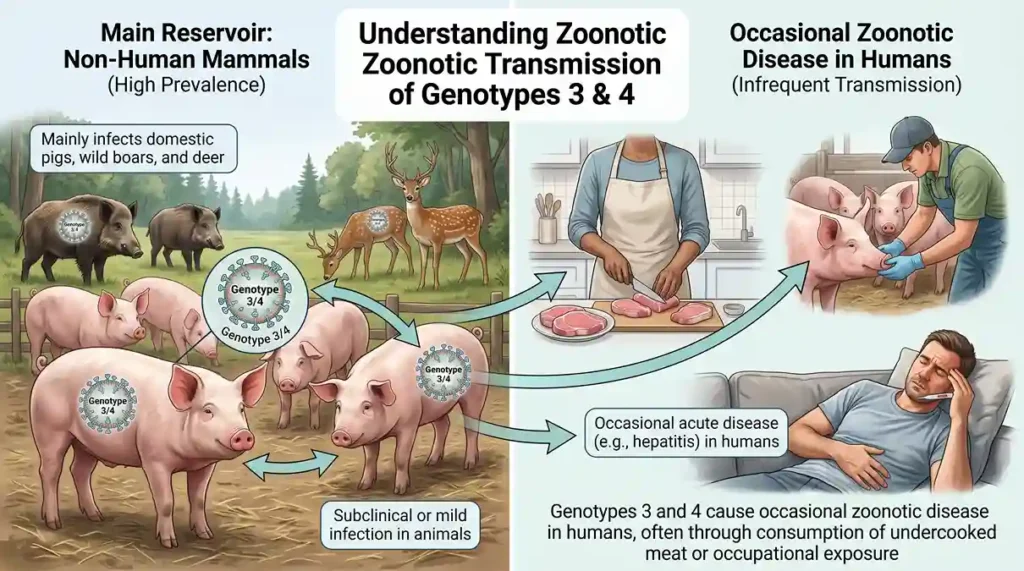
Genotypes 1 and 2 are primary viruses that can be transmitted to humans through contaminated water. While genotypes 3 and 4 do not directly transmit to humans. They primarily affect non-human mammals.
These genotypes can pose a risk of zoonotic diseases in humans through the consumption of raw or undercooked meat. Which means that hepatitis E is known to be transferable from animals to humans.
In Africa and many regions of Asia, genotypes 1 and 2 are the most commonly found forms of this virus.
Treatment of hepatitis E
Acute hepatitis E is typically self-limiting, and in most cases, hospitalization is not necessary; specific antiviral treatment is not yet available. The use of certain medications may impair liver function.
In specific conditions, this infection may require hospitalization for effective management, such as:
- A pregnant woman who is infected and exhibits signs and symptoms, especially during the second or third trimester. These women are at a high risk of developing acute liver failure and potential fetal demise. The World Health Organization reports that the mortality rate for women affected with hepatitis E can be as high as 20 to 25 percent during the third trimester of pregnancy.
- Patients with fulminant hepatitis, which is characterized by acute liver failure.
Prevention of hepatitis E
Transmission can be prevented through:
- Public water supplies with quality standards
- Proper disposal systems for human faeces.
- Maintaining and promoting hygienic conditions.
- The HEV 239 vaccine is currently available for hepatitis E. It protects high-risk populations and mitigates the occurrence of disease outbreaks.
What is the WHO response to viral hepatitis?
The World Health Organization’s Global Health Sector Strategy on HIV, Viral Hepatitis, and Sexually Transmitted Infections for the period 2022 to 2030 presents a comprehensive framework aimed at eliminating viral hepatitis as a significant public health concern.
This strategy is focused on achieving a 90% reduction in the spread of hepatitis and 65% reduction in mortality rates, compared to 2015.
FAQ
Disclaimer: This article is intended for educational and informational purposes only and should not be considered medical advice. Always consult a qualified healthcare professional for diagnosis and treatment.
References:
- CDC. (2024, April 1). Hepatitis C Basics. Hepatitis C. https://www.cdc.gov/hepatitis-c/about/index.html
- CDC. (2024, June 17). ABCs of Viral Hepatitis. Viral Hepatitis Awareness. https://www.cdc.gov/hepatitis-awareness/abcs/index.html
- CDC. (2024, May 14). Hepatitis D Basics. Hepatitis D. https://www.cdc.gov/hepatitis-d/about/index.html
- CDC. (2024, May 14). Hepatitis E Basics. Hepatitis E. https://www.cdc.gov/hepatitis-e/about/index.html
- CDC. (2024, May 9). Hepatitis A Basics. Hepatitis A. https://www.cdc.gov/hepatitis-a/about/index.html
- CDC. (2025, January 31). Hepatitis B Basics. CDC. https://www.cdc.gov/hepatitis-b/about/index.html
- Dagmara CZARSKA-THORLEY. (2020, May 26). Hepcludex – European Medicines Agency. European Medicines Agency. https://www.ema.europa.eu/en/medicines/human/EPAR/hepcludex
- EMA. (2018, September 17). Direct-acting antivirals indicated for treatment of hepatitis C (interferon-free). European Medicines Agency. https://www.ema.europa.eu/en/medicines/human/referrals/direct-acting-antivirals-indicated-treatment-hepatitis-c-interferon-free
- Hepatitis. (n.d.). www.who.int. https://www.who.int/health-topics/hepatitis
- New estimates highlight the need to step up the response to hepatitis D. (2026). Who.int. https://www.iarc.who.int/news-events/new-estimates-highlight-the-need-to-step-up-the-response-to-hepatitis-d/
- Office. (2024). MedWatch: Hepatitis C Medicines Drug Safety Communication. U.S. Food and Drug Administration. https://www.fda.gov/safety/medical-product-safety-information/hepatitis-c-medicines-mavyret-zepatier-and-vosevi-drug-safety-communication-due-rare-occurrence
- WHO. (2024, April 9). Hepatitis B. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/hepatitis-b
- WHO. (2024, July 15). Immunization Coverage. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/immunization-coverage
- World Health Organization. (2019, July 8). Hepatitis D. Who.int; World Health Organization: WHO. https://www.who.int/news-room/fact-sheets/detail/hepatitis-d
- World Health Organization. (2022, July 18). Global Health Sector Strategies. Www.who.int. https://www.who.int/teams/global-hiv-hepatitis-and-stis-programmes/strategies/global-health-sector-strategies
- World Health Organization. (2023, July 20). Hepatitis E. Who.int; World Health Organization: WHO. https://www.who.int/news-room/fact-sheets/detail/hepatitis-e
- World Health Organization. (2024, April 9). Hepatitis C. World Health Organization; World Health Organization: WHO. https://www.who.int/news-room/fact-sheets/detail/hepatitis-c
- World Health Organization. (2025, February 12). Hepatitis A. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/hepatitis-a