In today’s world, sexually transmitted infections (STIs) are a major public health concern globally. These infections affect people of all genders, ages, and socioeconomic backgrounds.
You might be thinking about many questions related to STIs, such as what are the most common sexually transmitted infections?. What is the difference between STIs and STDs? Which STIs are curable and which are not?. How to prevent STIs naturally and medically?. And can STIs be cured completely?
You will find all the answers about STIs in this detailed article.
Some infections are curable, while others are only manageable but not completely curable.
Infections can also be transmitted through the blood or from mother to baby during pregnancy or childbirth.
A sexually transmitted infection (STI) is the process of entrance of a pathogen in the human body, completion of its incubation period, and appearance of signs and symptoms.
As a result, a sexually transmitted disease (STD) is caused by the development of the infection through sexual contact.
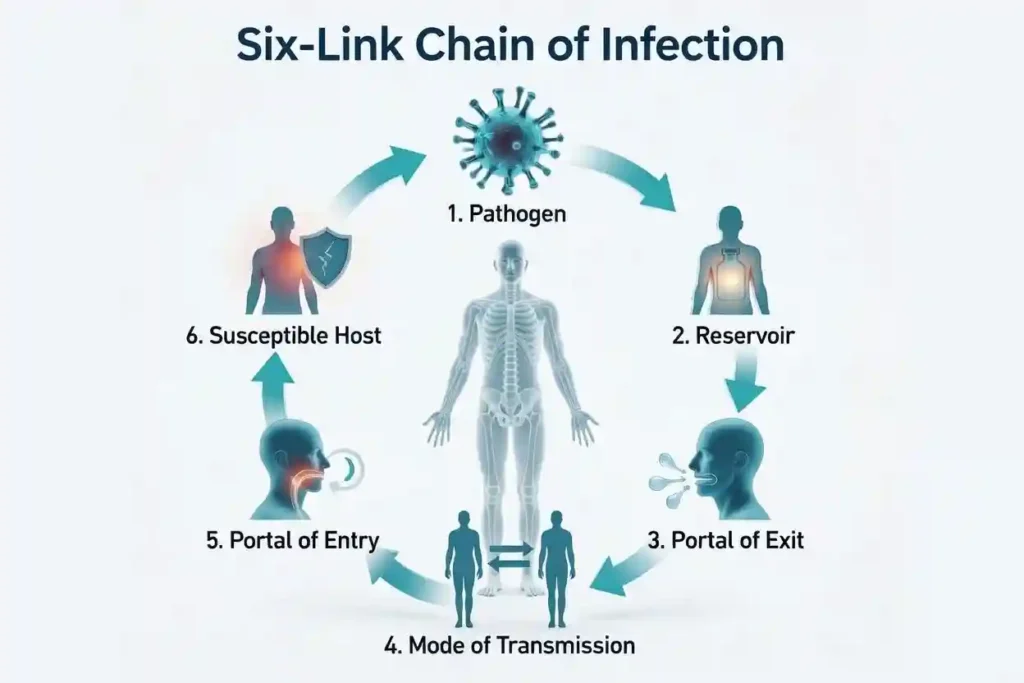
Understanding the six-link model chain of infection is crucial to understanding how infections spread from one person to another.
- This model starts with a “pathogen,” or infectious agent that causes the infection.
- The pathogen lives in a natural habitat where it grows or multiplies, and that natural habitat is called the “reservoir,” such as an animal, human, food, or water.
- From the reservoir, the pathogen requires a “portal of exit” to spread.
- After leaving the reservoir, the pathogen travels through a “mode of transmission.” This transmission may occur through the semen, secretions, air, or direct contact.
- After transmission, the pathogen enters a new person through a “portal of entry,” such as broken skin, mucous membranes, the respiratory tract, or ingestion.
- Finally, the pathogen infects a “susceptible host,” which can be a person who is at risk for getting an infection.
Sexually transmitted infections can be broadly categorized into three main types: bacterial, viral, and parasitic infections.
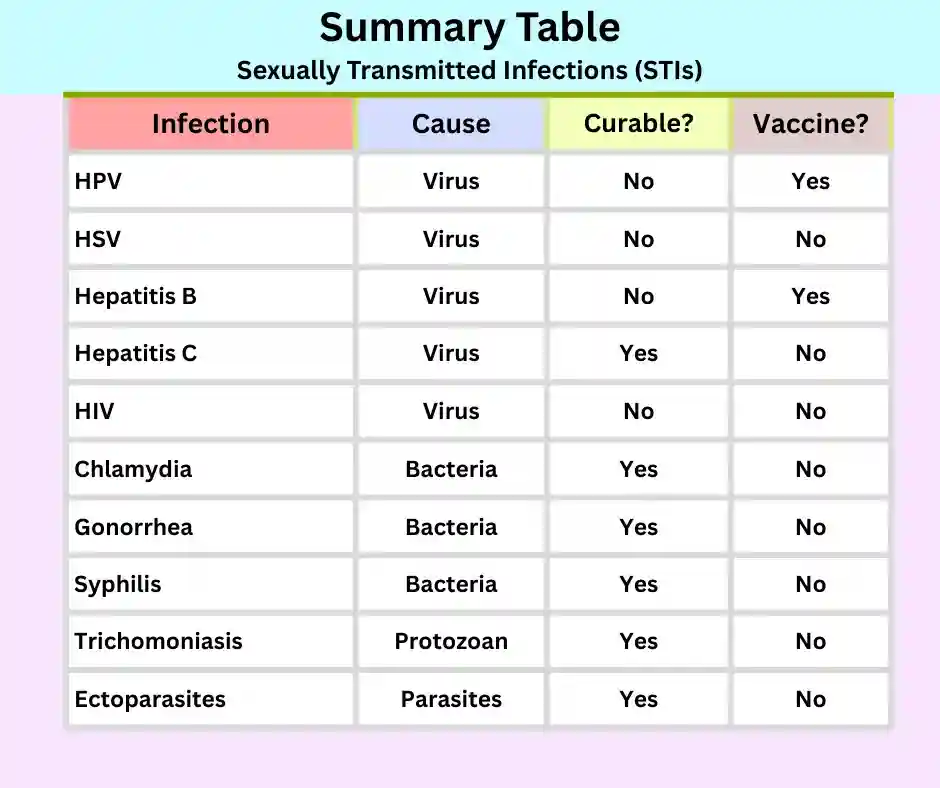
Common bacterial infections are curable with antibiotics; these infections include gonorrhea, syphilis, and chlamydia.
Viral infections include human immunodeficiency virus (HIV), human papillomavirus (HPV), herpes simplex virus, and viral hepatitis.
These infections are usually manageable but not completely curable.
The World Health Organization (WHO) has identified more than 30 pathogens that are transmissible through sexual contact.
For a quick review, which STIs are curable and which are not. See the STIs summary table.
Let’s reveal, what are the most common sexually transmitted infections.?

1. Human Papillomavirus (HPV)
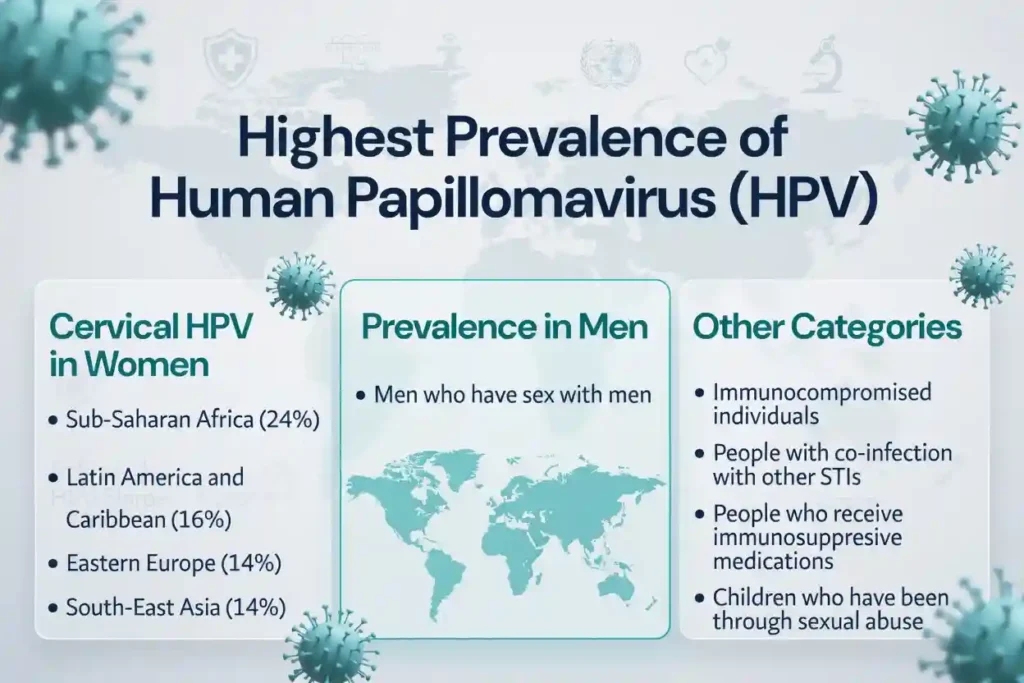
In the United States, there are many sexually transmitted infections, but human papillomavirus is one of the most common. About 70% of sexually active people acquire the HPV infection at any stage in their lives.
In many people, HPV can be cleared spontaneously within 3 years. However, repeated exposure to the virus can increase the risk of cancer.
According to the National Cancer Institute of the United States, human papillomavirus is actually a group of viruses, with more than 200 related viruses.
These viruses are divided into high-risk and low-risk types.
There are 12 types of high-risk viruses, of which HPV types 16 and 18 are responsible for causing most HPV-related cancers.
Low-risk types can also lead to cancers if not treated, but it is rare.
Human papillomavirus can cause cervical, anal, oropharyngeal, penile, vaginal, and vulvar cancers.
Every year, about 350000 women die from cervical cancer worldwide (WHO, 2024).
How does the human papillomavirus spread?
Human papillomavirus transmits between sexual partners through penile-vaginal sex, penile-anal sex, vaginal-oral sex, and penile oral sex.
What signs and symptoms can be seen in human papillomavirus?
Low-risk human papillomavirus may cause warts around the mouth, throat, anus, and genital areas.
While high-risk human papillomavirus is a dangerous infection, because it doesn’t show any signs or symptoms for many years, it depends on the location of the infection.
According to the World Health Organization, it usually takes 15 to 20 years for cervical cancer to develop after HPV infection.
Cervical cancer symptoms may include:
- Bleeding between menstrual periods.
- Bleeding after sexual intercourse.
- Foul-smelling vaginal discharge.
However, other factors may also lead to these symptoms.
How to prevent human papillomavirus?
Preventive measures include:
1. Vaccination
The first and most effective preventive measure against HPV is vaccination.
It is recommended that all girls aged 9 to 14 receive the vaccine for human papillomavirus prior to becoming sexually active (WHO,2024).
2. Screening
Women older than 30 years should be screened every 5 to 10 years for human papillomavirus (WHO,2024).
3. Protection
Use of condoms is recommended for the prevention of HPV, but it does not always ensure the prevention of transmission.
Male circumcision also reduces the risk of virus transmission.
What is the treatment for human papillomavirus?
There is currently no specific treatment available for the HPV infection itself. However, HPV-related cancers can be treated.
For cervical cancer, early detection is the most important factor for successful treatment.
Non-malignant and precancerous warts and lesions can be removed surgically or treated by ablation therapy.
2. Herpes Simplex Virus (HSV)
Herpes simplex virus, commonly known as “herpes,” is a highly contagious sexually transmitted infection.
Herpes is a chronic, lifelong infection. An infected person can transmit the virus, not only during the outbreak but also during the asymptomatic period.
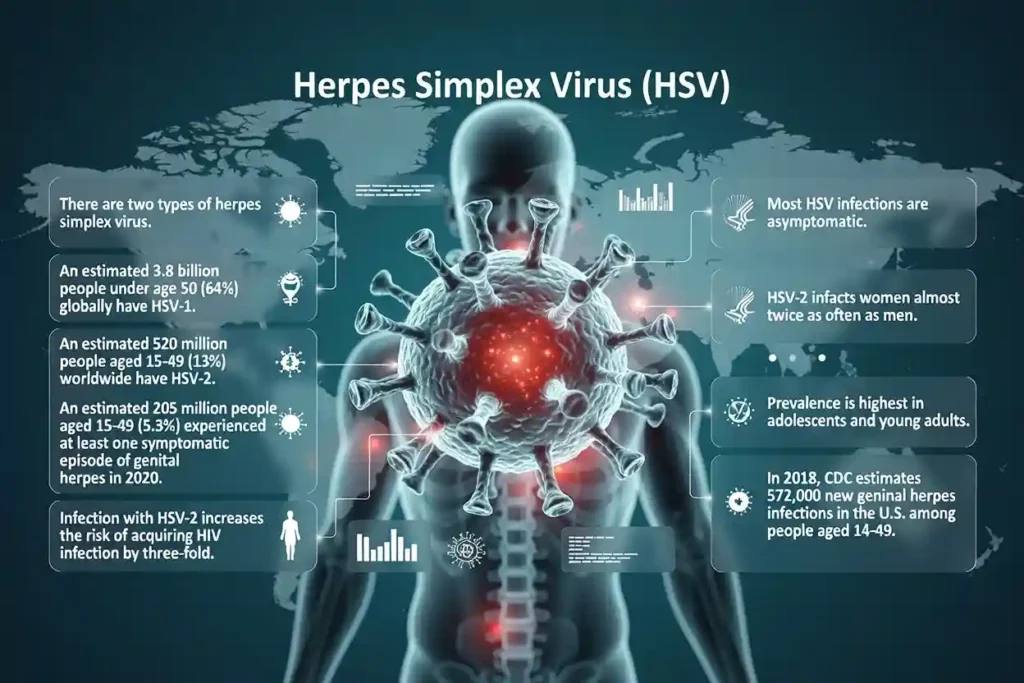
The herpes simplex virus (HSV) is classified into two distinct types. The first type is HSV-1, and the second is HSV-2.
According to the World Health Organization, in 2025, about 3.8 billion people worldwide had HSV-1, under the age of 50, representing 64% of the global population.
About 520 million people, representing 13% of the global population, had HSV-2 worldwide, aged 15 to 49 years.
How does the herpes simplex virus spread?
HSV-1, also known as oral herpes, spreads through oral contact between partners, such as from the genitals to the mouth and from mouth to mouth.
This infection usually appears around the mouth, commonly known as cold sores.
HSV-2 transmits through sexual intercourse. It causes the painful genital blisters, known as genital herpes.
Intrapartum transmission occurs when HSV-2 infection is transmitted from a pregnant woman to a neonate. It can cause permanent neurological damage or the neonate’s death.
The presence of HSV-2 also increases the risk of HIV transmission.
What are the signs and symptoms of HSV-1 and HSV-2 infections?
Most people remain asymptomatic or have mild symptoms. They remain unaware of the infection, which can lead to unintentional transmission to others.
Common symptoms include:
- Painful blisters
- Fever
- Headache
- Body pain
- Swelling of lymph nodes
These symptoms begin with burning of the sore site, itching, and tingling. People may experience some discharge and then crust over the blisters.
What is the treatment of herpes simplex virus?
Herpes simplex virus is a treatable condition but not curable. The first-line treatment of HSV is medicine. Antiviral and pain relief medications are often used for the treatment.
How can you prevent the herpes simplex virus?
For sexually active people:
- The use of a condom can significantly decrease the risk of genital herpes transmission. However, it does not completely ensure safety due to the presence of HSV in the anal and oral areas. These areas can come into contact with exposed body parts.
- Limiting the number of sex partners.
- Male circumcision can provide partial protection against the HSV-2 infection.
3. Viral Hepatitis
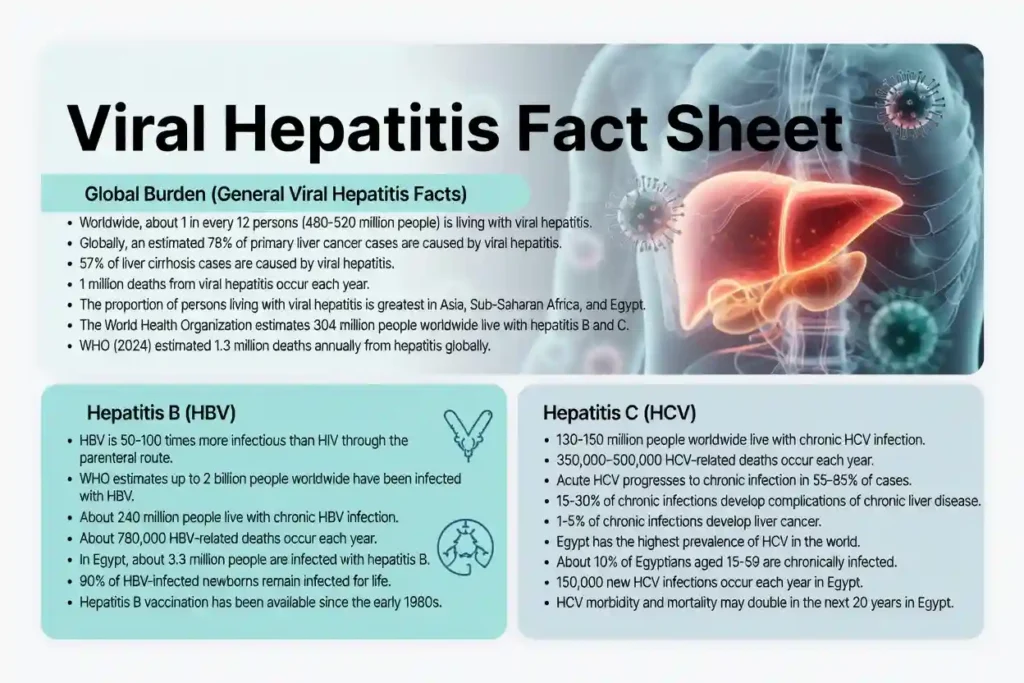
There are five types of viral hepatitis. Hepatitis A, B, C, D, and E. All these types are damaging to the liver.
These types are different in terms of severity, mode of transmission, prevention, treatment, and geographical distribution.
The World Health Organization estimates that 304 million people worldwide live with hepatitis B and C.
In 2024, the WHO reported that, every year, approximately 1.3 million deaths occur globally due to hepatitis infections.
How can viral hepatitis be transmitted from one person to another?
Viral hepatitis can be transmitted through many routes; some of them are sexually transmitted.
According to the Centers for Disease Control and Prevention (CDC):
- Hepatitis A can spread through certain sexual practices with an infected person having hepatitis A, especially among men, although the primary transmission route is contaminated food or water.
- Hepatitis B is transmitted through exposure to blood, semen, and various other bodily fluids.
- Hepatitis C is mainly transmitted through blood, but in some cases it can spread through sexual contact, particularly if a partner is HIV-positive or during anal sex.
- It can remain asymptomatic until advanced liver disease develops.
What signs and symptoms appear in viral hepatitis?
CDC reports that the signs and symptoms of all viral hepatitis present similarly.
Some of these are:
Nausea, stomach pain, jaundice, dark urine, clay-colored stool, fatigue, fever, joint pain, and loss of appetite.
Diarrhea occurs only in hepatitis A infection.
How to prevent and treat viral hepatitis?
Universal preventive measures for viral hepatitis include:
- Limiting the number of sexual partners.
- Use of condoms.
However, these strategies do not eliminate the risk of viral hepatitis.
- Hepatitis A is preventable with vaccination and avoidance of sexual contact with a person having an active infection. If someone is exposed to hepatitis A, physicians usually recommend proper rest, nutrition, and fluids to treat the infection.
- Hepatitis B is also preventable with vaccination. CDC reports that hepatitis B is manageable but not curable. Currently, there is no specific medicine to treat the hepatitis B virus.
- There is no vaccine for the hepatitis C virus, but HCV is treatable and permanently curable in 95% of people without significant signs and symptoms. The usual duration of therapy is approximately 8 to 12 weeks.
The Food and Drug Administration (FDA) approved medicine list is available on the website of “Hepatitis C Online.”
4. Human Immunodeficiency Virus (HIV) and AIDS
Human immunodeficiency virus, or HIV, is one of the most serious sexually transmitted infections because it damages the immune system.
HIV attacks CD4 T-cells, gradually weakening the body’s ability to fight against infections and cancers.
Untreated HIV infection can progress to acquired immunodeficiency syndrome (AIDS), which is the most advanced stage of the disease.
According to World Health Organization data from 2024, approximately 40.8 million people were living with HIV worldwide, and 630,000 people died from HIV related causes that year.

How can HIV be transmitted to others?
Human immunodeficiency virus can spread through blood, sharing contaminated needles, semen, rectal and vaginal fluids, and breast milk. Transmission may also occur from a mother to her newborn.
According to the World Health Organization, HIV does not spread from kissing, hugging, or sharing food.
The quantity of a virus in the bloodstream is referred to as the viral load.
CDC reports that viral load is crucial in the transmission of the virus to others. When viral load becomes undetectable in blood, the virus cannot be transmitted through sex, childbirth, or sharing drug needles.
What signs and symptoms can be seen in HIV patients?
The signs and symptoms of HIV can differ based on the specific stage of the infection. CDC defines 3 stages of HIV.
Some people may not experience any symptoms, while others may experience flu-like symptoms within 2 to 4 weeks after exposure, which can persist for up to 10 weeks.
However, these symptoms do not indicate a positive HIV infection. Testing and screening are the most authentic ways to detect human immunodeficiency virus.
Stage 1
Stage 1, the acute stage, may cause flu-like symptoms, including fever, headache, rash, and sore throat.
Stage 2
In the chronic stage, or stage 2, CD4 cells decline, viral load increases, and the immune system progressively weakens. People may experience weight loss, fever, diarrhea, cough, and swollen lymph nodes.
Some people may not experience any symptoms or get sick.
Stage 3
Stage 3, or late-stage, is characterized by severe immunosuppression, where the CD4 cell count drops below 200 cells/mm³ or less than 14% CD4 cells. This condition progresses to AIDS.
At this stage, people may acquire opportunistic infections, such as tuberculosis, severe bacterial infections, cryptococcal meningitis, and certain types of cancer.
How to prevent HIV?
HIV is preventable and manageable, but not completely curable.
Preventive strategies include:
- Never to share drug injection items like syringes or needles.
- Routine STI testing.
- Use of male and female condoms during sex.
- Male circumcision.
- Use of pre-exposure prophylactic antiretroviral therapy, before exposure to HIV, or post-exposure prophylactic antiretroviral therapy after exposure to HIV.
What is the treatment of HIV?
The World Health Organization reports there is no cure for HIV infection. Antiretroviral drugs reduce the replication of the virus, which allows the body to strengthen its immune system.
Ultimately, these antiretroviral drugs reduce the viral load in the blood, and people can live a healthy life.
People with an undetectable viral load are also unable to transmit the virus to others.
5. Chlamydia Trachomatis
“Chlamydia trachomatis” is the causative bacterium of chlamydia.
It is often asymptomatic, which contributes significantly to its widespread transmission.
According to the Centers for Disease Control and Prevention, chlamydia is the most common bacterial sexually transmitted infection in the United States, with approximately 2.8 million new cases reported every year.
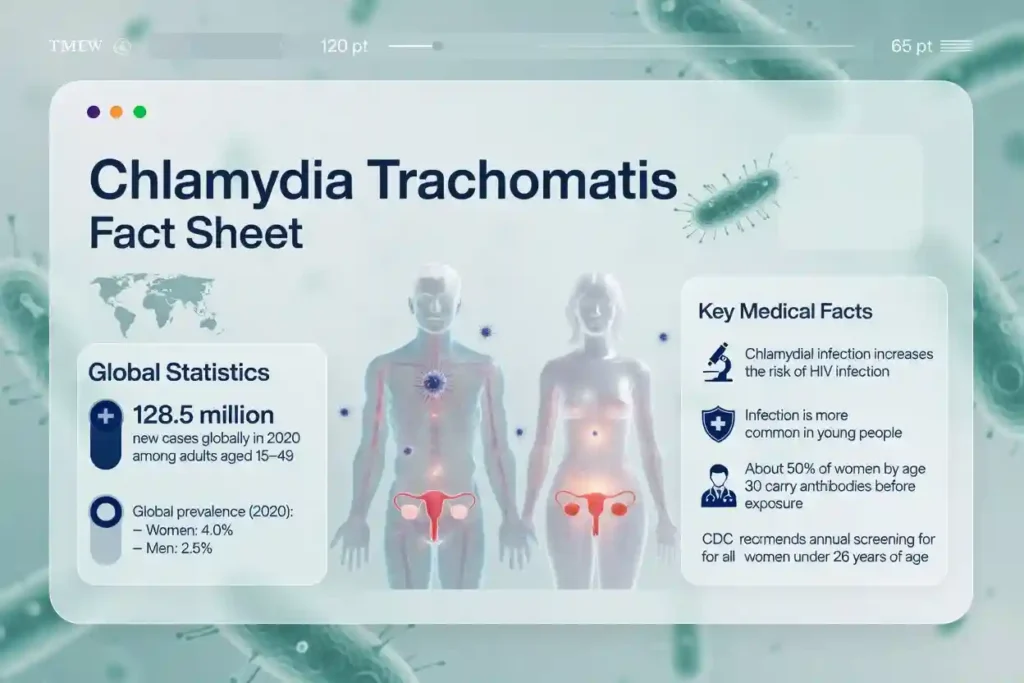
It is estimated that about 50% of women by the age of 30 have antibodies indicating previous exposure.
The World Health Organization reported 128.5 million new cases in 2020 among people aged 15 to 49 years globally.
How does chlamydia spread?
Chlamydia spreads through oral, anal, or vaginal sex with an infected partner, especially when a condom is not used.
An infected mother can also transmit the infection to her baby during the process of childbirth.
What clinical signs and symptoms are seen in chlamydia infection?
Chlamydia often causes no symptoms, and many people remain unaware that they are infected.
Symptoms may appear several weeks after exposure.
In women, symptoms may include:
- An abnormal vaginal discharge
- A burning sensation during urination
- Pain after sexual intercourse
- Itching and lower abdominal pain
- Bleeding between menstrual cycles
Men can experience:
- Discharge from the penis
- Pain during urination
- Swelling in the testes in some cases
Rectal infection can occur in both men and women, and may cause pain, discharge, and bleeding.
How to prevent a chlamydial infection?
Currently, there is no vaccination available for chlamydia infection.
The CDC recommends annual screening for all sexually active women under the age of 26.
Testing during pregnancy is also important to prevent the transmission of infections from mother to baby.
Using condoms correctly during sexual activity and limiting the number of sexual partners also reduces the risk of infection.
What are the treatment options for chlamydia infection?
Chlamydia is easily diagnosed using laboratory tests and is curable and treatable with antibiotics.
Untreated chlamydia can lead to significant complications, including infertility, pelvic inflammatory disease, and ectopic pregnancy.
6. Gonorrhea
Gonorrhea is caused by “Neisseria Gonorrhoeae”.
It is the second most common bacterial STI reported in the United States and is very common among young adults aged 15 to 24 years.
According to the World Health Organization, approximately 82.4 million cases were reported globally in 2020 among people aged 15 to 49 years.
The WHO also reports that gonococcal infection increases the risk of HIV transmission by five times.

How does gonorrhea spread?
Gonorrhea usually spreads through oral, vaginal, and anal sex with an infected person.
What signs and symptoms appear in gonorrhea?
Many individuals may remain asymptomatic.
In women, symptoms may include:
- Painful urination
- Thick vaginal discharge
- Vaginal bleeding between menstrual periods
Symptoms in men may include:
- Burning sensation during urination.
- Penile discharge may present in various colors, including white, yellow, or greenish.
- Swelling in the testicles occurs in rare cases.
Rectal symptoms are similar in men and women, including anal itching, discharge, bleeding, soreness, and painful bowel movements.
What is the prevention of gonorrhea?
Currently, no vaccine is available for gonorrhea.
Preventive strategies include:
- Correct and consistent use of condoms during sexual activity.
- Sustaining a monogamous relationship for a long time with a partner who is not infected.
- The CDC recommends annual screening for sexually active individuals under 25, as well as for older individuals with risk factors or multiple sexual partners.
- It is also recommended that pregnant women undergo screening for gonorrhea.
How to treat gonorrhea?
Gonorrhea is a treatable and curable infection.
Treatment typically involves cephalosporin antibiotics.
However, both CDC and WHO have raised their concerns about increasing drug-resistant strains of gonorrhea.
It reflects that the bacterium is becoming stronger every day, making treatment increasingly challenging.
7. Syphilis
Syphilis is a bacterial infection. It progresses through distinct stages.
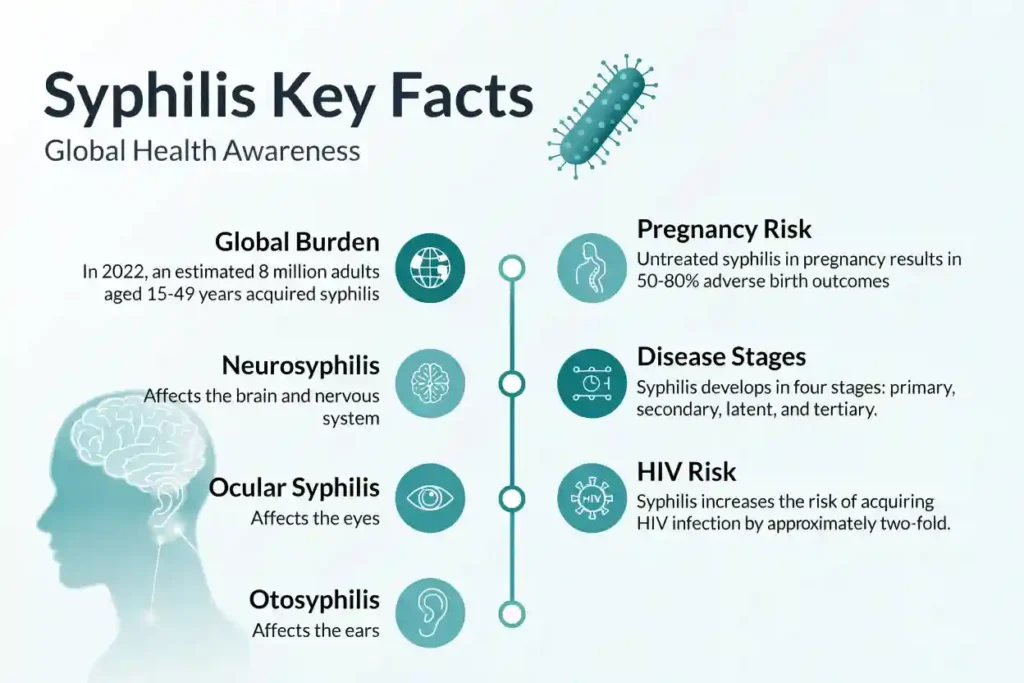
The CDC defines four stages of syphilis:
- Primary stage
- Secondary stage
- Latent stage
- Tertiary stage
Every stage presents with different signs and symptoms.
According to the World Health Organization, approximately 8 million people aged 15 to 49 acquired syphilis in 2022.
How does syphilis spread to others?
Syphilis is a highly contagious disease.
CDC reported that syphilis can be transmitted through anal, vaginal, or oral sex and contact with casual objects such as swimming pools, doorknobs, bathtubs, hot tubs, toilet seats, and sharing eating utensils and clothing.
Pregnant women can pass syphilis to their babies during birth.
What signs and symptoms are noted in syphilis?
Primary stage
In the primary stage, one sore or multiple sores appear on the site where syphilis enters the body. These sores usually appear on the vagina, penis, anus, lips, or mouth.
Sores can be painless, round, and firm. People do not notice these sores because of their painless characteristic; even healthcare providers can miss them.
These sores heal in 3 to 6 weeks regardless of treatment, but infection remains present in the body.
If you don’t get treatment, the infection goes to the secondary stage.
Secondary stage
In the secondary stage, Symptoms may include rough, red, or reddish brown sores or rashes on multiple areas of the body.
These sores can be seen during or after the healing of primary sores.
People may experience fever, headache, sore throat, muscle ache, tiredness, and patchy hair loss.
Without proper treatment, this stage progresses to the latent or tertiary stage.
Latent stage
During the latent stage, no symptoms appear, but the infection remains present and may last for years without treatment.
When symptoms appear, it can be fatal; this condition is known as the tertiary stage.
Tertiary stage
The tertiary stage does not develop in the majority of people.
However, when it appears, it can affect different body organ systems, including the heart, blood vessels, brain, and nervous system.
Tertiary syphilis can occur after 10 to 30 years of initial infection.
When syphilis affects the nervous system, it is called neurosyphilis, which may cause severe headaches, changes in mental status, dementia, or muscle weakness.
When the infection affects the eyes, it is called ocular syphilis, which can lead to eye pain, redness, vision changes, and even blindness.
Otosyphilis is a condition in which infection affects the ears. The patient may experience vertigo, dizziness, and tinnitus, which means buzzing, ringing, or roaring in the ears.
What are the preventive measures for syphilis?
There is no vaccine available for syphilis.
Correct use of a condom during every sexual encounter is the best strategy. But safety is not always ensured by using condoms because syphilis can spread through uncovered areas such as the genitals or mouth.
Having sex with a single sexual partner also reduces the risk of syphilis.
The WHO recommends annual testing for sexually active individuals and screening for all pregnant women.
What are the treatment options for syphilis?
The World Health Organization recommends Benzathine Penicillin G as the primary treatment for early and latent syphilis.
It is also recommended for pregnant women to prevent transmission of syphilis to babies.
Healthcare providers also use other antibiotics such as doxycycline, ceftriaxone, or azithromycin,
8. Trichomoniasis
Trichomoniasis is caused by a protozoan parasite called Trichomonas vaginalis, and is one of the most common non-viral sexually transmitted diseases.
According to the CDC, more than 2 million cases were reported in the United States in 2018.
Globally, the World Health Organization reported 156 million new cases by 2020.
CDC also reports that trichomoniasis is more common in women than in men, and older women are more likely to be infected than younger women.

What signs and symptoms appear in trichomoniasis infection?
It is estimated that around 70% of individuals who are infected remain asymptomatic.
Symptoms in men may include:
- Itching inside the penis.
- Burning after ejaculation or urination.
- Penile discharge.
In women, symptoms may include:
- Redness and itching in the genital area.
- Burning sensation.
- Fishy-smelling vaginal discharge that may be white, yellow, or greenish.
How does trichomoniasis spread?
Trichomoniasis spreads through sexual contact without the use of condoms.
Parasite transmits:
- From penis to vagina
- From the vagina to penis
What is Prevention of Trichomoniasis?
No vaccine is available for trichomoniasis.
The same strategies are useful as in syphilis, such as using a condom correctly, having a single sex partner, and being tested for sexually transmitted infections.
Is trichomoniasis treatable?
Trichomoniasis is one of the most easily curable sexually transmitted infections. It is usually treated with antibiotics such as metronidazole or tinidazole.
9. Sexually Transmitted Ectoparasites
Some sexually transmitted conditions are caused not by microorganisms but by parasites living on the skin.
These include:
- Pubic lice, medically known as pediculosis pubis, are caused by a parasite, Phthirus pubis.
- Scabies is a skin infection caused by an ectoparasite, Sarcoptes scabiei
How do ectoparasites spread?
These parasites usually spread through close physical or sexual contact with an infected person.
What are the signs and symptoms of ectoparasites?
- In cases of pubic lice, you may notice visible lice and eggs, known as nits, in the pubic region. The person may have intense itching in the pubic area.
- In scabies, tiny burrows, mites, eggs, and mite feces may be present in the skin, causing severe itching.
Are ectoparasites preventable?
Sexual contact should be avoided if signs or symptoms of infection are present.
Open communication and disclosure between sexual partners also reduces the risk of transmission.
How to get rid of ectoparasites?
Centers for Disease Control and Prevention (CDC) recommends the treatment for both scabies and pubic lice.
Pubic lice can be treated with oral and topical regimens.
Primary treatments:
- Permethrin 1% cream rinse applied to all affected areas.
- Pyrethrin with piperonyl butoxide is applied to all affected areas.
Alternative treatments:
- Malathion 0.5% lotion is applied to all affected areas.
- Ivermectin 250 micrograms per kilogram of body weight orally.
Scabies can also be treated with both oral and topical regimens.
Primary treatments:
- Permethrin 5% cream is applied to every part of the body from the neck down.
- Ivermectin 200 micrograms per kilogram of body weight orally.
Alternative treatments:
- Lindane 1%, one ounce of lotion or 30 grams of cream, applied in a thin layer to all areas of the body from the neck down
Lindane is not recommended for infants or children under 10 years of age.
Future implications for overcoming sexually transmitted infections?
Sexually transmitted infections are preventable and manageable with the right knowledge and care. They represent a diverse group of infections with varying causes, symptoms, and outcomes.
While many STIs are curable, others require lifelong management and can lead to serious health consequences if left untreated.
Education, routine testing, vaccination, early treatment, and safer sexual practices remain the most effective strategies for reducing the burden of sexually transmitted infections and protecting public health.
The World Health Organization has proposed a global vision to eliminate sexually transmitted diseases by the year 2030.

To achieve this goal, the WHO introduced the Global Health Sector Strategies for 2022 to 2030.
The core objectives and targets of this initiative are:
- Reducing the number of new cases.
- Preventing mother-to-child transmission of diseases such as congenital syphilis, HIV, and hepatitis B.
- Providing vaccines.
- Expanding screening for pregnant women and priority populations.
- Monitoring and reporting antimicrobial resistance (AMR).
To achieve these targets and objectives, the WHO developed the Five Strategic Directions framework.
- The first strategic direction focuses on providing high-quality, people-centered services.
- The second focuses on optimizing interventions to achieve maximum impact.
- The third emphasizes strengthening surveillance and data collection to understand epidemic trends and guide decision-making.
- The fourth encourages engagement of civil society and empowerment of communities.
- The fifth promotes innovation for greater impact.
However, the WHO progress report published in 2024 highlighted several challenges in achieving these targets.
These challenges include:
- Global shortages of essential medicines
- Rapidly increasing antimicrobial resistance
- Access to diagnostic tests is often limited in resource-limited settings.
A mid-term review of the strategy is scheduled for 2026 to evaluate global progress.
Reference List
- About Chlamydia. (2025, January 31). Chlamydia. https://www.cdc.gov/chlamydia/about/index.html
- About gonorrhea. (2025, January 31). Gonorrhea. https://www.cdc.gov/gonorrhea/about/index.html
- About HIV. (2025, January 14). HIV. https://www.cdc.gov/hiv/about/index.html
- About syphilis. (2025, January 30). Syphilis. https://www.cdc.gov/syphilis/about/index.html
- About trichomoniasis. (2025, January 31). Trichomoniasis. https://www.cdc.gov/trichomoniasis/about/index.html
- Chain of infection components. (n.d.). https://www.cdc.gov/niosh/learning/safetyculturehc/module-2/3.html
- Chlamydial Infections – STI treatment Guidelines. (n.d.). https://www.cdc.gov/std/treatment-guidelines/chlamydia.htm
- Clinical overview of viral hepatitis. (2025, August 29). Viral Hepatitis. https://www.cdc.gov/hepatitis/hcp/clinical-overview/index.html
- Data on syphilis. (2025, September 10). https://www.who.int/data/gho/data/themes/topics/data-on-syphilis
- Ectoparasitic Infections – STI treatment Guidelines. (n.d.). https://www.cdc.gov/std/treatment-guidelines/ectoparasitic.htm
- Global health sector strategies on HIV, viral hepatitis and sexually transmitted infections for the period 2022-2030. (2022, July 18). https://www.who.int/publications/i/item/9789240053779
- Global health sector strategies. (n.d.). https://www.who.int/teams/global-hiv-hepatitis-and-stis-programmes/strategies/global-health-sector-strategies
- HPV and Cancer. (2025, May 9). Cancer.gov. https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv-and-cancer
- Medications to treat HCV – treatment –. (n.d.). Hepatitis C Online. https://www.hepatitisc.uw.edu/page/treatment/drugs
- Neisseria gonorrhoeae. (n.d.). https://www.who.int/teams/immunization-vaccines-and-biologicals/diseases/neisseria-gonorrhoeae
- Principles of Epidemiology: Lesson 5, Appendix B|Self-Study Course SS1978|CDC. (n.d.). https://archive.cdc.gov/www_cdc_gov/csels/dsepd/ss1978/lesson5/appendixb.html
- Viral hepatitis among sexually active adults. (2024, May 14). Viral Hepatitis. https://www.cdc.gov/hepatitis/hcp/populations-settings/sexually-active.html
- World Health Organization: WHO & World Health Organization: WHO. (2025, May 30). Herpes simplex virus. https://www.who.int/news-room/fact-sheets/detail/herpes-simplex-virus
- World Health Organization: WHO & World Health Organization: WHO. (2025b, July 15). HIV and AIDS. https://www.who.int/news-room/fact-sheets/detail/hiv-aids
- World Health Organization: WHO & World Health Organization: WHO. (2025c, November 21). Chlamydia. https://www.who.int/news-room/fact-sheets/detail/chlamydia
- World Health Organization: WHO & World Health Organization: WHO. (2025c, October 22). Gonorrhoea (Neisseria gonorrhoeae infection). https://www.who.int/news-room/fact-sheets/detail/gonorrhoea-(neisseria-gonorrhoeae-infection)
- World Health Organization: WHO & World Health Organization: WHO. (2025a, May 29). Syphilis. https://www.who.int/news-room/fact-sheets/detail/syphilis
- World Health Organization: WHO. (2020c, March 11). Hepatitis. https://www.who.int/health-topics/hepatitis
- World Health Organization: WHO. (2025, September 10). Sexually transmitted infections (STIs). https://www.who.int/news-room/fact-sheets/detail/sexually-transmitted-infections-(stis)
- World Health Organization: WHO. (2025b, December 2). Cervical cancer. https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
- World Health Organization: WHO. (2025b, October 22). Multi-drug resistant gonorrhoea. https://www.who.int/news-room/fact-sheets/detail/multi-drug-resistant-gonorrhoea
- World Health Organization: WHO. (2025c, November 21). Trichomoniasis. https://www.who.int/news-room/fact-sheets/detail/trichomoniasis
Understanding STIs is crucial for public health awareness.
Many people have questions about STIs and their impact on health.
Being informed about STIs can help in prevention and treatment.
STIs can be categorized based on their causative agents.
Awareness of common STIs helps in early detection and management.
Regular testing for STIs is essential for sexually active individuals.
Communication between partners about STIs is vital for prevention.
Strategies to prevent STIs should be discussed with healthcare providers.
Education about STIs can reduce transmission rates significantly.
STIs are a focus for global health initiatives and research.
STIs require continuous public health efforts to control outbreaks.
Reducing new cases of STIs should be a primary healthcare goal.
Understanding STIs contributes to overall community health.
STIs can have serious health implications if not addressed promptly.
Regular discussions about STIs in relationships can enhance sexual health.
Preventive measures against STIs should be a priority for all sexually active individuals.
Outreach programs focused on STIs can help educate the public.
STIs remain a significant topic in sexual health education.
Awareness campaigns about STIs can improve community health outcomes.